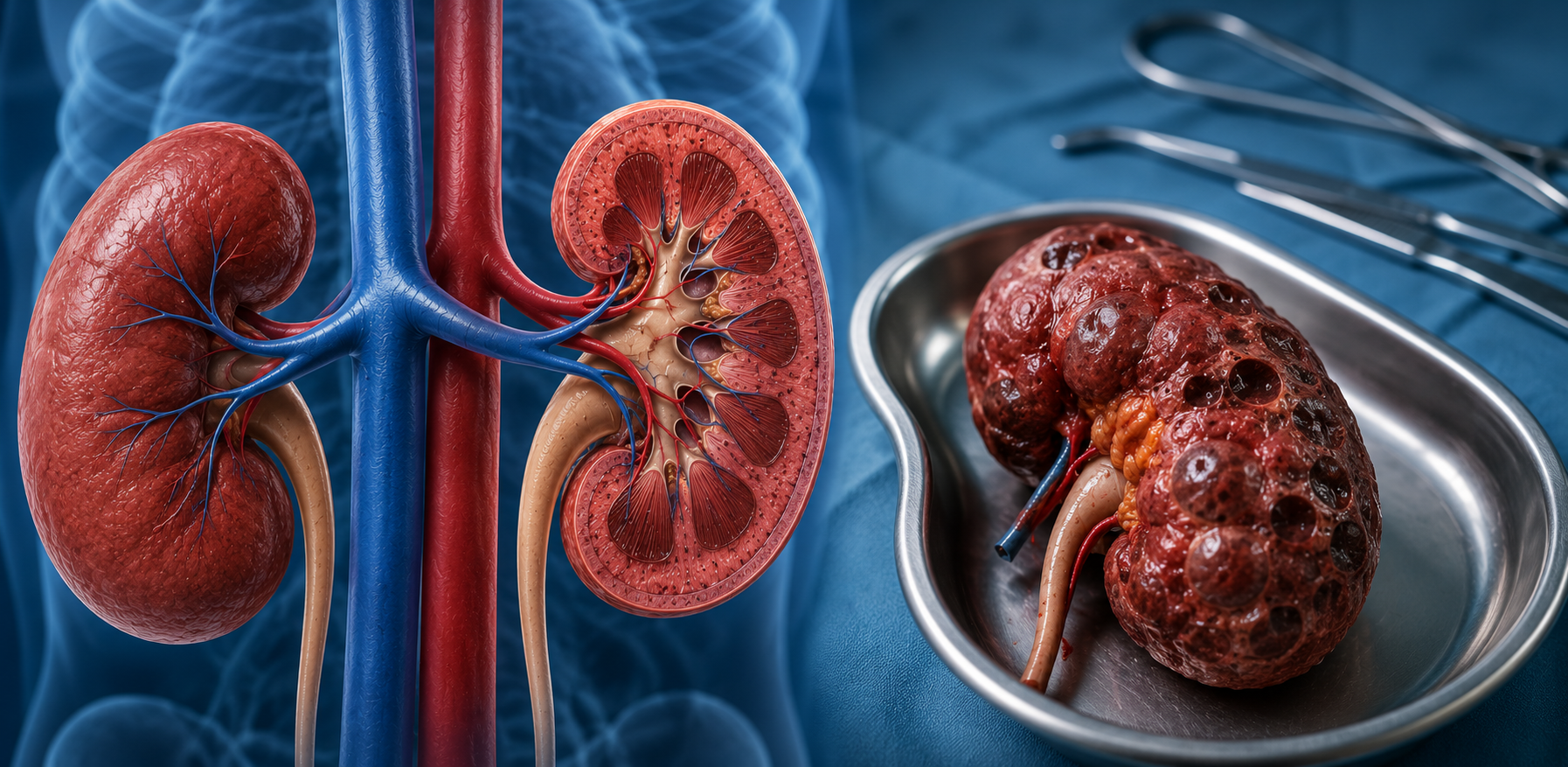
Chronic kidney infections are often underestimated until they progress to irreversible damage. Among these, chronic pyelonephritis stands out as a condition that can quietly deteriorate renal function over months or years. In advanced cases, the affected kidney may lose functionality entirely – leaving surgical removal, or nephrectomy, as the only viable treatment.
Recent clinical observations and published case reports highlight how delayed diagnosis and persistent infection can lead to this outcome, emphasizing the importance of early intervention and structured management.
Understanding Chronic Pyelonephritis
Chronic pyelonephritis is a long-term inflammatory disorder of the kidney caused by recurrent or persistent bacterial infections. Unlike acute infections, which present with sudden and severe symptoms, chronic cases develop gradually and are often linked to structural abnormalities or urinary obstruction.
Over time, repeated inflammation leads to renal scarring, tubular atrophy, interstitial fibrosis, and progressive loss of kidney function.
Evidence from studies indexed by the National Institutes of Health shows that untreated or poorly managed infections can permanently alter renal architecture, ultimately resulting in functional decline (read the full study on PubMed Central).
Why Do Kidneys Become Non-Functional?
A kidney becomes non-functional when its filtration capacity is severely compromised. This is typically the result of prolonged pathological processes such as chronic infection, obstructive uropathy, hydronephrosis (urine accumulation causing swelling), renal calculi, and vesicoureteral reflux.
Clinical insights suggest that obstruction combined with infection accelerates tissue destruction. In such cases, even interventions like drainage procedures may fail to restore function. A detailed clinical overview is available in this urology article on acute pyelonephritis.
Further supporting research can be explored through studies published on ScienceDirect and Oxford Academic (OFID).
Clinical Presentation: Subtle but Progressive
One of the challenges in managing chronic pyelonephritis is its often non-specific presentation. Patients may experience persistent dull flank pain, recurrent fever episodes, fatigue, dysuria, and occasionally hematuria.
As renal function declines, symptoms become more pronounced. However, by this stage, significant and often irreversible damage may already have occurred.
Case Insight: Chronic Pyelonephritis Leading to Nephrectomy
A case report published in the Journal of Pharmaceutical Research International provides a clear illustration of disease progression and management (read the full case report here).
Patient Profile
A 45-year-old male presented with a four-month history of abdominal pain localized to the left loin region, radiating toward the back. The pain was insidious, intermittent, and progressively worsening.
The patient had previously undergone percutaneous nephrostomy (PCN) for severe hydronephrosis. Despite initial intervention, symptoms persisted and renal function continued to decline.
Diagnostic Evaluation
The diagnostic workup included ultrasonography and contrast-enhanced computed tomography (CECT).
Imaging findings confirmed gross hydronephrosis, severe structural damage, and a non-functioning left kidney. These findings indicated irreversible renal impairment, making surgical intervention necessary.
Nephrectomy: Indications and Rationale
Nephrectomy, the surgical removal of a kidney, is typically considered when the risks of retaining a diseased organ outweigh its benefits.
Common indications include non-functioning kidney, chronic infection resistant to treatment, severe obstruction, recurrent stone disease, traumatic injury, and malignancy.
In cases of chronic pyelonephritis, nephrectomy helps eliminate the source of infection, prevent systemic complications, and relieve persistent pain.
Surgical Management and Post-Operative Care
In the reported case, the patient underwent a left simple nephrectomy. Post-operative management focused on infection control, pain relief, and gastrointestinal protection.
Treatment included broad-spectrum antibiotics such as piperacillin–tazobactam, metronidazole for anaerobic coverage, proton pump inhibitors like pantoprazole, antiemetics such as ondansetron, and analgesics including tramadol and paracetamol.
Close monitoring ensured stabilization and minimized the risk of complications.
Outcome and Recovery
The patient demonstrated a favorable recovery trajectory, with complete resolution of pain, no post-operative complications, and stable clinical parameters.
This case reinforces that timely surgical intervention in advanced chronic pyelonephritis can lead to excellent outcomes when combined with appropriate medical care.
Living with a Single Kidney
Following nephrectomy, most individuals can lead normal and healthy lives with one functioning kidney. However, long-term care is essential.
Patients are advised to maintain adequate hydration, monitor blood pressure, undergo regular kidney function tests, avoid nephrotoxic medications, and follow a balanced diet.
Clinical evidence suggests that a single healthy kidney can effectively compensate for the loss of the other.
Prevention and Clinical Implications
Preventing chronic pyelonephritis depends largely on early detection and proper management of underlying conditions.
Key strategies include prompt treatment of urinary tract infections, management of urinary obstruction, monitoring high-risk patients such as those with diabetes, and regular imaging in recurrent cases.
From a clinical perspective, this condition highlights the importance of timely diagnosis, imaging, and intervention to prevent irreversible renal damage.
Conclusion
Chronic pyelonephritis remains a clinically significant condition with the potential to progress to irreversible kidney damage. When a kidney becomes non-functional, nephrectomy serves as a definitive and often necessary treatment.
The presented case underscores the importance of early diagnosis, structured management, and timely surgical decision-making in improving patient outcomes.
As research continues to evolve, emphasis on preventive care and early intervention remains essential in reducing the burden of chronic kidney disease.
Reference
- National Institutes of Health. (n.d.). Chronic pyelonephritis and renal infection study. PubMed Central.
https://pmc.ncbi.nlm.nih.gov/articles/PMC13097013/ - Dr. Soarawee Urology. (2021, April 2). Acute pyelonephritis.
https://drsoaraweeurology.com/2021/04/02/acute-pyelonephritis/ - Elsevier. (2026). Article on renal infection and complications. ScienceDirect.
https://www.sciencedirect.com/science/article/abs/pii/S0735675726000823 - Oxford University Press. (2026). Study published in Open Forum Infectious Diseases.
https://academic.oup.com/ofid/article/13/1/ofaf748/8417038 - Morey, S. G., Sharma, R., & Ghungrud, D. (n.d.). Nephrectomy in patient of chronic pyelonephritis with non-functioning kidney on left side: A case report. Journal of Pharmaceutical Research International.
https://journaljpri.com/index.php/JPRI/article/view/4850